VAGAL NERVE STIMULATION IN EPILEPSY
 Vagus nerve stimulation (VNS) is designed to
prevent seizures by sending regular, mild pulses of
electrical energy to the brain via the vagus nerve.
These pulses are supplied by a device something like
a pacemaker.
Vagus nerve stimulation (VNS) is designed to
prevent seizures by sending regular, mild pulses of
electrical energy to the brain via the vagus nerve.
These pulses are supplied by a device something like
a pacemaker.
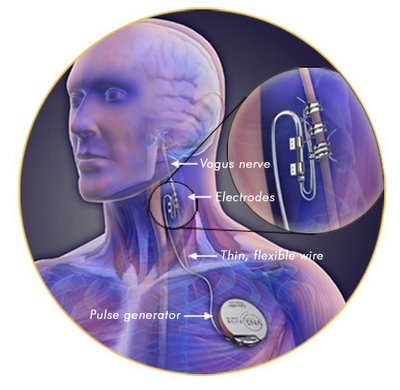
The VNS device is sometimes referred to as a
"pacemaker for the brain." It is placed under the
skin on the chest wall and a wire runs from it to
the vagus nerve in the neck.
The vagus nerve is part of the autonomic nervous
system, which controls functions of the body that
are not under voluntary control, such as the heart
rate. The vagus nerve passes through the neck as it
travels between the chest and abdomen and the lower
part of the brain.
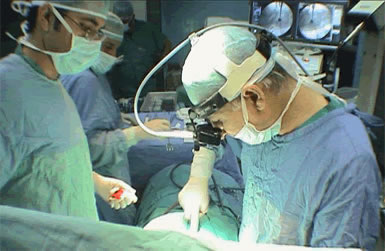
 What is the surgery like?
What is the surgery like?
The surgeon first makes an incision along the outer
side of the chest on the left side, and the device
is implanted under the skin. Then a second incision
is made horizontally in the lower neck, along a
crease of skin, and the wire from the stimulator is
wound around the vagus nerve in the left side of the
neck. The brain itself is not involved in the
surgery.
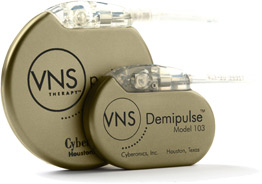
The device (also called an implant) is a flat, round
battery, about the size of a silver dollar—that is,
about an inch and a half (4 cm) across—and 10 to 13
millimeters thick, depending on the model used.
Newer models may be somewhat smaller.
| |
 |
 |
|
| |
Fig. 1 Cyberonics batteries |
Fig. 2 VNS Implant diagram. |
|
The procedure usually lasts about 50 to 90 minutes
with the patient under general anesthesia. Sometimes
a hospital stay of one night is required. Some
surgeons have performed the procedure with local
anesthesia and the patient has been discharged the
same day.
 How is VNS used?
How is VNS used?
The neurologist programs the strength and timing of
the impulses according to each patient's individual
needs. The settings can be programmed and changed
without entering the body, just by using a
programming wand connected to a laptop computer.
For all patients, the device is programmed to go on
for a certain period (for example, 7 seconds or 30
seconds) and then to go off for another period (for
example, 14 seconds or 5 minutes). The device runs
continuously, usually with 30 seconds of stimulation
alternating with 5 minutes of no stimulation. The
patient is usually not aware that it's operating.
Holding a special magnet near the implanted device
causes the device to become active outside of the
programmed interval. For people with warnings
(auras) before their seizures, activating the
stimulator with the magnet when the warning occurs
may help to stop the seizure. Many patients without
auras also experience improved seizure control,
however.
 Settings (also called stimulation parameters)
set by the neurologist typically include a
stimulation amplitude of 1.0 to 3.0 mA
(milliamperes), a stimulation frequency of 30 Hz
(hertz), and a pulse width of 500 microseconds. By
adjusting these settings, the doctor not only may be
able to control more of the patient's seizures, but
often can also relieve side effects. One study, for
instance, found that changing the pulse width
eliminated pain that some patients were
experiencing.
Settings (also called stimulation parameters)
set by the neurologist typically include a
stimulation amplitude of 1.0 to 3.0 mA
(milliamperes), a stimulation frequency of 30 Hz
(hertz), and a pulse width of 500 microseconds. By
adjusting these settings, the doctor not only may be
able to control more of the patient's seizures, but
often can also relieve side effects. One study, for
instance, found that changing the pulse width
eliminated pain that some patients were
experiencing.
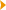 The battery for the stimulator lasts approximately
5-10 years
The battery for the stimulator lasts approximately
5-10 years |